Harpenden Stadiometer Manual Meat
Subjects/Methods:This study used data on 4750 mother–offspring pairs, collected as a part of the Avon Longitudinal Study of Parents and Children, Bristol, UK between 1991 and 1992; associations between behavioural exposures occurring from conception up to 5 years of age (maternal and paternal smoking during pregnancy, breastfeeding, age at introduction to solids, dietary patterns and physical inactivity during early childhood) and offspring body composition measured by dual-energy X-ray absorptiometry at 15 years were assessed. Results:After full adjustment for potential confounders, maternal smoking during pregnancy, having a junk food diet and spending more time watching television in early childhood were all associated with higher fat mass at age 15, whereas maternal smoking, having a healthy diet and playing computer games more frequently in early childhood were all associated with a higher lean mass at age 15. Associations with paternal smoking were generally weaker for both fat and lean mass, but as there was no strong statistical evidence for maternal vs paternal differences, confounding by social factors rather than a direct effect of maternal smoking cannot be ruled out. Early feeding was not associated with fat or lean mass at age 15. IntroductionThe prevalence of overweight and obesity has rapidly increased in recent years, and according to the latest Health Survey for England, 63% of adults (aged 16 or over) and 30% of children (aged 2–15) are overweight or obese. Obese children and adolescents have been found to have risk factors for cardiovascular disease such as hyperlipidemia, hypertension and abnormal glucose tolerance, as well as an increased risk of asthma, hepatic steatosis, sleep apnoea and type 2 diabetes.
Longer-term risks include adult obesity, ischaemic stroke, joint disease, cancer and coronary heart disease, in addition to the chronic conditions mentioned above.,It has been suggested that fetal life, infancy and early childhood may be particularly sensitive periods for predicting obesity. Many previous studies have investigated the role of early-life (from conception to 5 years of age) risk factors for later obesity and overweight, and Monasta et al. Have undertaken a review of published systematic reviews of these studies.
In addition, Reilly et al. Investigated 25 potential early-life risk factors for obesity at age seven in the Avon Longitudinal Study of Parents and Children (ALSPAC).
These studies were mainly based on body mass index (BMI) which is known not to be a good measure of adiposity as it cannot distinguish between fat and lean mass, and few recorded the outcomes in adolescents.Body composition data, that is, fat and lean mass derived from dual-energy X-ray absorptiometry at 15 years old are now available in ALSPAC. Therefore the objective of this study was to use ALSPAC to investigate whether associations between a number of behavioural early-life exposures and body composition at age 15 years exist. The choice of early-life exposures was based on those identified from the Monasta and Reilly papers which are available within ALSPAC and considered to be behavioural and therefore have the potential to be modified. They include parental smoking in pregnancy, early feeding (breastfeeding and age at introduction of solids), dietary patterns in early childhood (derived using principal components analysis), and physical inactivity in early childhood (time spent in the car, watching television and playing computer games). For all analyses, the effect of confounding was explored by adjustment for a wide range of potentially confounding factors in regression models. In addition, for smoking, the associations between maternal and paternal exposures and the outcomes were compared; a stronger association observed with maternal compared with paternal smoking is more likely to represent a causal intrauterine influence, whereas similar associations with both maternal and paternal smoking suggest that confounding by family level environment and/or genetic factors is a likely explanation.
Sample and study designALSPAC is a geographically based birth cohort investigating the health and development of children, which is described in detail elsewhere. Briefly, all pregnant women living in three health districts of Bristol (formerly known as the Avon Health Area), UK with expected delivery dates between 1 April 1991 and 31 December 1992 were eligible to take part in the study. A total of 14 541 were enrolled and 13 678 had a singleton, live born child.
The 'Harpenden' range of anthropometric instruments, which have been developed in close collaboration with the University of London Institute of Child Health, are counter recording and they give accurate and direct readings to the nearest millimetre.
Detailed data have been collected by self-completed questionnaires (relating to the mother, her partner and her offspring) from pregnancy onwards. From the age of seven, all children have been invited to regular research clinics. Ethical approval was obtained from the ALSPAC Ethics and Law Committee and the Local Research Ethics Committees. The study website contains details of all the data that are available through a fully searchable data dictionary. Early-life exposure variablesA list of all early-life exposure variables and the time point of measurement is shown in.
At enrolment, the mother was asked whether her partner was the father of her unborn child. All variables relating to the partner were set to missing if the mother answered ‘no' or ‘not sure', or did not answer this question, to allow estimation of the contribution of factors that are potentially shared (either through genetics or environment) between father and offspring. In the 18-week antenatal questionnaire, the mother was asked whether she smoked tobacco (1) in the first 3 months of pregnancy and (2) in the past 2 weeks.
Positive responses (cigarettes, cigars, pipes or ‘other') were grouped together to create dichotomous variables to represent smoking in the first and second trimesters, respectively. In the 32-week antenatal questionnaire, the mother was asked how many cigarettes she was currently smoking per day, and this was categorized into a dichotomous variable to represent smoking in the third trimester. Responses from the three trimesters were combined to create a variable for any smoking during pregnancy. In the 18-week-gestation questionnaires, both the mother and father were asked if he had smoked regularly over the past 9 months; the father's response was used if available, otherwise the mother's response about the father was used.
From the 6-month maternal questionnaire, a variable was derived for exclusive breastfeeding, coded as exclusive breastfeeding beyond 2 months of age, partial breastfeeding (breastfeeding had been stopped or was non-exclusive by 2 months) and never breastfed. Exclusive breastfeeding was defined as no solids, milk formulas or other drinks, except vitamins, minerals, medicines and/or water. The mother was also asked to record the age in months when her child was introduced to solids, which was grouped into ⩽2, 3 and ⩾4 months of age.When the child was 38 months old, the mother was asked to complete a food frequency questionnaire about their eating habits. Outcome variables at age 15At the 15-year clinic visit, total fat and total lean mass were measured using a Lunar Prodigy DXA scanner (GE Medical Systems Lunar, Madison, WI, USA); the scans were visually inspected and any automated sectioning that did not match the true body sections was manually realigned. Height was measured with shoes and socks removed using a Harpenden stadiometer (Holtain Ltd, Crymych, Pembrokeshire, UK), and weight was measured using a Tanita TBF 305 body fat analyser and weighing scales (Tanita United Kingdom Ltd., Yewsley, Middlesex, United Kingdom); from these BMI was calculated as weight (in kilos) divided by height squared (in metres). Potential confounding factorsAt enrolment, the mother was asked to record her parity, height and pre-pregnancy weight, and BMI was calculated from these. The father was asked to record his height and weight (used to calculate BMI).
The 32-week antenatal questionnaire asked the mother to record her highest education level which was then categorized into none/CSE (national school exams at age 16), vocational, O level (national school exams at age 16, higher than CSE), A level (national school exams at age 18) or university degree. At this time, she also recorded the occupation of both herself and the father; the lowest was used to allocate them to social class groups (classes I (highest occupational social class) to V (lowest)) using the 1991 OPCS (Office of Population Censuses and Surveys) classification. The mother's age at delivery was calculated from the date of delivery and the mother's date of birth recorded at enrolment. The estimation of gestation was based on the date of the last menstrual period reported by the mother. Offspring gender and birthweight were recorded in the delivery room and abstracted from obstetric records and/or birth notifications.Children were sent a puberty questionnaire, which included questions on developmental stage after they had made an appointment for the 15-year clinic visit with the intention that they completed it before their appointment. Pubertal stage for males was based on pubic hair development and for females was based on the most advanced stage for pubic hair and breast development; data were set to missing if the puberty questionnaire was not completed within 16 weeks of the dual-energy X-ray absorptiometry scan (this was only the case for two children). Free 3d java game download for touch screen pc.

Statistical analysesMeans and s.d. Were calculated for continuous variables that were approximately normally distributed, medians and interquartile ranges for skewed variables (fat mass and BMI at 15 years only), and proportions for categorical variables. Further analysis was based on internally derived s.d.
Scores for total fat mass, lean mass and BMI to allow comparison of the regression coefficients between the outcome measures. These were calculated by subtracting the mean from the individual's value, then dividing by the s.d.; the mean and s.d. Were based on the whole sample. Logged fat mass and logged BMI were used to calculate the s.d.
Scores due to the skewness of the distribution.Associations between each of the exposures (maternal smoking, paternal smoking, breastfeeding, age at introduction to solids, four dietary patterns at 38 months, time spent in the car at 38 months, time spent watching television at 38 months and frequency of playing computer games at 57 months) and the main outcomes (fat mass s.d. Score, lean mass s.d.
Score) were assessed using linear regression. For each of the 11 exposures, adjustment was first made for gender and age at the time of body composition measurement (plus energy intake at 38 months for the four dietary patterns; Model 1), then additionally for parental factors (maternal and paternal height, maternal and paternal BMI, maternal age, parity), social factors (social class, maternal education) plus birthweight and gestation (Model 2). All the models were adjusted for height to take into account differences in stature.As well as separate models with maternal or paternal smoking as the exposure, additional models were fitted with maternal and paternal smoking variables included simultaneously; statistical tests were used to compare the maternal and paternal regression coefficients.
Also, even though paternal data were set to missing if the mother had not confirmed her partner to be the true biological father of her child, a sensitivity analysis was carried out to assess the potential effects of various possible rates of unknown non-paternity of partners on the results for parental smoking; for fully adjusted simultaneous models; the Clemons command in STATA, was used.Associations in males and females separately were compared by including interaction terms for gender and exposure variables in the models. The minimally adjusted models were repeated restricting to those with complete confounder information, to ensure that any changes in regression coefficients were attributable to confounding rather than missing data. The fully adjusted models were repeated with additional adjustment for pubertal status. Finally, models were repeated with BMI s.d. Score as the outcome. All the analyses were performed in Stata version 12.1 (StataCorp, College Station, TX, USA).
ResultsData on 5112 were available from the 15-year clinic visit. Analysis was based on the 4750 with at least one early-life exposure plus offspring body composition at age 15. Partner data were set to missing for 2.4% of the 4634 with at least one variable recorded, as the partner had not been confirmed as the biological father of the child. And, display the summary data for all the exposures (except factor loadings for dietary patterns at 38 months), outcomes and potential confounders. For interpretation of the regression coefficients generated from the models below, s.d. Were 0.6 kg on the logarithmic scale for fat mass, and, as shown in, 8.4 kg for lean mass (0.16 kg m −2 for BMI). NMeans.d.OutcomesFat mass at 15-year clinic visit (kg)475013.78.3, 20.1Lean mass at 15-year clinic visit (kg)475043.18.4BMI (kg m −2)474520.719.0, 23.0ConfoundersMaternal height (cm)4560164.46.7Maternal pre-pregnancy BMI (kg m −2)433722.83.7Paternal height (cm)3472176.56.8Paternal BMI at time of pregnancy (kg m −2)344825.13.2Maternal age in pregnancy (years)475029.24.5Gestation (weeks)475039.51.8Birthweight (kg)46893.40.5Energy intake at 38 months (kJ per day)4280.1Age at 15-year clinic visit (years)475015.50.3Height at 15-year clinic visit (cm)4748169.38.4.
Minimally adjustedFully adjustedβ(95% CI)P -valueβ(95% CI)P -valueOutcome=fat mass at 15 years (s.d. Score)SeparatelyMaternal smoking0.160.09, 0.22. EFor interpretation, lean mass 0.7 kg higher, if mother smoked.Maternal and paternal smoking were both associated with higher fat mass at age 15 after minimal adjustment for confounders, and the effect sizes were similar. After full adjustment for potential confounders, the association with maternal smoking remained, whereas that with paternal smoking was weakened; however, there was no statistical evidence for a difference in associations ( P=0.6). Refitting the minimally adjusted models restricting to those with complete confounder data only, or adding pubertal status to fully adjusted models made little difference to the findings (see ).
In the fully adjusted simultaneous model also adjusted for a hypothetical non-paternity rate as high as 20%, the associations with paternal smoking strengthened, whereas those with maternal smoking remained similar (see; P=0.3–0.8 for differences in associations between maternal and paternal smoking).Maternal smoking was more strongly associated with higher lean mass at age 15 years than paternal smoking, although the statistical evidence for a difference was not strong ( P=0.02 for the minimally adjusted model, P=0.1 for the fully adjusted model). Again, findings were similar after restricting minimally adjusted models to those with complete confounder information only, or adding pubertal status to fully adjusted models (see ). Adjusting for non-paternity made little difference to the findings (see ). Feeding in infancy, and diet and physical inactivity in early childhoodAssociations between each of the exposures in infancy/early childhood and fat and lean mass at age 15 are shown in; there were no interactions with gender for any of these exposures ( P0.1 for all). Although several exposures (not breastfeeding, earlier age at introduction to solids, eating more junk food, eating less healthy food, more time spent in the car and more time spent watching television) were associated with higher fat mass at 15 years after only minimal adjustment, once all potential confounders were included in the models the only associations that remained were with the junk dietary pattern and time spent watching television. Separate modelsMinimally adjustedFully adjustedβ(95% CI)P -valueβ(95% CI)P- valueOutcome=fat mass at 15 years (s.d. BAdditionally adjusted for parental factors, social factors, birthweight and gestation.There was only modest evidence for higher lean mass at age 15 if more time was spent playing computer games (before and after adjustment for potential confounders).
All exposuresAll the 11 exposures were then included in fully adjusted models simultaneously. The findings were generally similar to those of the separate fully adjusted models ( and ). Maternal smoking, the junk dietary pattern and time spent watching television were all associated with higher fat mass at age 15. Maternal smoking, the healthy dietary pattern and playing computer games were all associated with a higher lean mass at age 15; the inverse association with the junk pattern was substantially weakened when all the exposures were considered simultaneously. The association with maternal smoking was stronger for fat mass than for lean mass, and although for both outcomes, associations with paternal smoking were weaker than for maternal smoking, there was no statistical evidence of a difference ( P=0.3 for fat mass and P=0.2 for lean mass). Simultaneous fully adjusted modelsOutcome=fat mass at 15 years (s.d. Score)Outcome=lean mass at 15 years (s.d.
AAdjusted for gender, age at the time of 15-year clinic visit, height, parental factors, social factors, birthweight and gestation (plus energy intake at 38 months for dietary patterns).As shown in, 18.5% of the mothers smoked at some point during pregnancy. Considering each trimester separately, 17.0% smoked in the first, 13.2% in the second and 12.6% in the third trimester, with only 7.2% changing their smoking habits during pregnancy. For both fat and lean mass, associations were almost identical to the combined smoking variable for the first and second trimesters, whereas the association was marginally stronger for the third trimester (see; simultaneous adjustment for all exposures).Finally, all the 11 exposures were included in fully adjusted models simultaneously, but with BMI s.d. Score as the outcome.
No early-life factors were clearly associated with BMI at age 15; the apparent association between maternal smoking in pregnancy and higher BMI was not found to be statistically different from the association with paternal smoking ( P=0.2). DiscussionThis study, on the basis of a large, contemporary cohort, has examined associations between behavioural factors occurring between conception and 5 years of age, and directly measured fat and lean mass at age 15, taking into account a wide range of potential confounders. Maternal smoking during pregnancy, having a junk food diet and spending more time watching television at approximately age three were all associated with higher fat mass at age 15. Maternal smoking, having a healthy diet at approximately age three and playing computer games more frequently at approximately five were all associated with a higher lean mass at age 15.
Associations with paternal smoking were generally weaker than those for maternal smoking for both fat and lean mass at age 15, but as there was no strong statistical evidence for maternal vs paternal differences, confounding by social factors rather than a direct effect of maternal smoking cannot be ruled out (see Taylor et al. For an explanation of the maternal/paternal negative control approach). Early feeding (breastfeeding and age at introduction to solids) was not associated with fat or lean mass at age 15 after adjusting for confounders.The main strengths of the current study are its size, the direct measurement of body composition and the rigorous analyses undertaken such as adjustment for a wide range of confounders and assessment of the potential effects of non-paternity when comparing maternal and paternal effects. However, this study also has a number of limitations. It is possible that different results would have been obtained if all children whose mothers originally enrolled in the study were able to be included in the analysis. However, only modest differences in most characteristics can be seen between those in the current analysis, and those who did not attend the clinic. In addition, findings were similar if the minimally adjusted analyses were restricted to those with complete data on all confounders rather than including any with available data, providing some reassurance that attrition is unlikely to have biased results.The smoking data were self-reported by mothers and their partners, however, a meta-analysis of comparisons between biochemical measures and self-reported smoking found the self-reported data to be accurate.
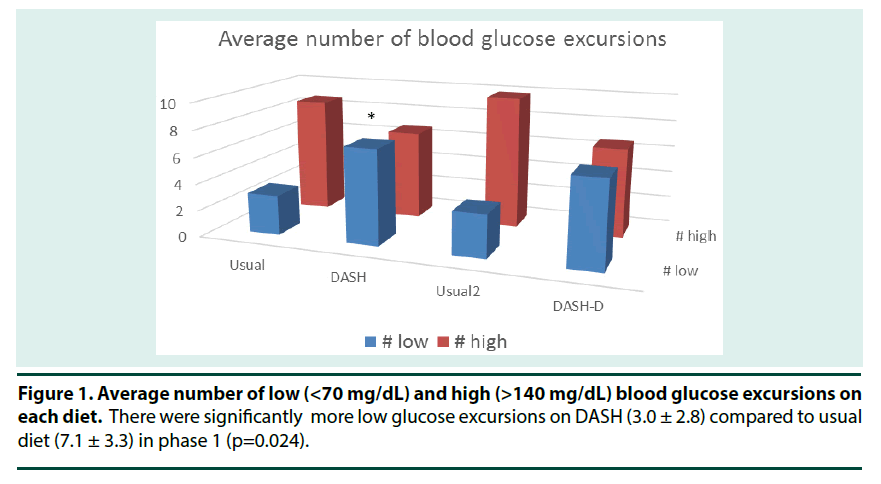
Early feeding data were also self-reported, but recall bias should have been minimal as the information was obtained from the mothers regularly throughout early infancy. Due to the large number of subjects, it was necessary to use unquantified food frequency questionnaires to assess diet in early childhood. Although food frequency questionnaires are a less accurate method of dietary assessment than using weighed dietary records, they have been shown to provide a reasonable measure of diet in large cohorts and may, in fact, estimate intakes of less commonly eaten foods more accurately than dietary records. The physical inactivity variables were reported by mothers which was not ideal, but there was no robust practical method of objectively measuring physical activity/inactivity on large numbers of young children within the epidemiological setting.We have demonstrated associations between maternal smoking and offspring fat and lean mass at age 15 years, although as there is no statistical evidence that associations with maternal smoking are stronger than those with paternal smoking, confounding is a likely explanation. Although many studies have demonstrated associations between maternal smoking during pregnancy and offspring overweight and obesity (for example, Reilly et al. And relevant reviews from Monasta et al.
), to our knowledge, the only previous study to investigate associations between both maternal and paternal smoking and fat or lean mass in the offspring was also based on ALSPAC, with outcomes assessed at an earlier age when the children were 10 years old. Although it is not possible to directly compare the effect sizes between these two studies (as internally derived s.d. Scores are not comparable as the variation in body composition widens as children get older), overall conclusions were similar.We did not find any associations between breastfeeding or the age at introduction to solids and fat or lean mass at age 15 after adjustment for confounders. Previous studies have reported inconsistent associations between breastfeeding and offspring overweight/obesity at various ages (for example, Reilly et al.
And several reviews identified by Monasta et al. ), however, the general pattern seems to be that any observed associations are substantially weakened or removed after adjustment for confounding factors. A small number of studies have investigated breastfeeding and dual-energy X-ray absorptiometry measured body composition in adolescence, and most did not find associations with either fat mass, or lean mass, in offspring aged between 16 and 18 years after adjusting for confounders.
Further evidence that there is no causal association is provided by a randomized breastfeeding promotion intervention in Belarus which did not reduce child obesity.Despite the large number of studies addressing the issue of breastfeeding and offspring obesity, very few have investigated associations with the age at introduction of solids, and these are mainly limited to BMI in childhood as the outcome. Yang and Huffman and Przyrembel have reviewed the existing evidence and concluded that findings were mixed, and adjustment was not always made for confounders. In addition, Reilly et al.
Did not observe an association between the age at introduction to solids and BMI at age seven in ALSPAC.We have demonstrated positive associations between having a junk food diet at age three and increased fat mass at age 15, and between having a healthy diet at age three and increased lean mass at age 15; no associations between other dietary patterns in early childhood (healthy, traditional, fussy/snack) and offspring fat mass/BMI were observed. Although Reilly et al. Found an association between the junk food diet at age three and BMI in 5-year-old ALSPAC children, to our knowledge, there are no studies investigating these types of dietary patterns in early childhood and adolescent body composition.We have found increased time spent watching television and time spent playing computer games in early childhood to be associated with increased fat mass and increased lean mass at age 15, respectively, whereas there were no associations with time spent in the car in early childhood. Reilly et al. Have shown time spent watching television but not time spent in the car to be associated with BMI at 5 years in ALSPAC, and also relevant reviews from Monasta et al. (52 studies assessing time spent watching television and six assessing time spent playing computer games) showed associations with BMI at age 3–18 years. To our knowledge, no studies have investigated associations between these physical inactivity variables in early childhood and offspring fat or lean mass.
Our observed association between increased time spent playing computer games in infancy and lean mass in adolescence is difficult to explain and may be a chance finding, so requires replication.So in conclusion, this study does not provide compelling evidence that parental smoking or early feeding are associated with directly measured body composition in adolescence. There is some suggestion that associations with dietary patterns and physical inactivity in early childhood may exist, but further studies are required to confirm our findings in different cohorts, particularly as our study is one of the first to examine associations with directly measured body composition in adolescence. If associations with these early-life exposures are shown to exist, the future direction of research should then focus on whether these deleterious effects can be overcome by improved diet and physical activity in adolescence. We are extremely grateful to all the families who took part in this study, the midwives for their help in recruiting them and the whole ALSPAC team, which includes interviewers, computer and laboratory technicians, clerical workers, research scientists, volunteers, managers, receptionists and nurses. This publication is the work of the authors and Sam Leary, Debbie Lawlor, George Davey Smith, Marie-Jo Brion and Andy Ness will serve as guarantors for the contents of this paper.
This work was supported by the European Union 6th framework programme, Early Nutrition Programming Project EARNEST (FOOD-CT-2005-007036). The UK Medical Research Council and the Wellcome Trust (Grant ref: 092731) and the University of Bristol provide core support for ALSPAC.
Health Survey for England: Reducing Obesity and Improving Diet Policy. (accessed 24 April 2013). Dietz WH, Gortmaker SL. Preventing obesity in children and adolescents. Annu Rev Public Health2001; 22: 337–353. Gaziano JM.
Fifth phase of the epidemiologic transition: the age of obesity and inactivity. JAMA2010; 303: 275–276.
August GP, Caprio S, Fennoy I, Freemark M, Kaufman FR, Lustig RH et al. Prevention and treatment of pediatric obesity: an endocrine society clinical practice guideline based on expert opinion. J Clin Endocrinol Metab2008; 93: 4576–4599. Gardner DS, Hosking J, Metcalf BS, Jeffery AN, Voss LD, Wilkin TJ. Contribution of early weight gain to childhood overweight and metabolic health: a longitudinal study (EarlyBird 36).
Pediatrics2009; 123: e67–e73. Monasta L, Batty GD, Cattaneo A, Lutje V, Ronfani L, Van Lenthe FJ et al. Early-life determinants of overweight and obesity: a review of systematic reviews. Obes Rev2010; 11: 695–708. Reilly JJ, Armstrong J, Dorosty AR, Emmett PM, Ness A, Rogers I et al. Early life risk factors for obesity in childhood: cohort study.
BMJ2005; 330: 1357. Wells JC. A critique of the expression of paediatric body composition data. Arch Dis Child2001; 85: 67–72. Smith GD. Assessing intrauterine influences on offspring health outcomes: can epidemiological studies yield robust findings?
Basic Clin Pharmacol Toxicol2008; 102: 245–256. Golding J, Pembrey M, Jones R, Team AS.
ALSPAC-the Avon Longitudinal Study of Parents and Children. Study methodology. Paediatr Perinat Epidemiol2001; 15: 74–87. Brion MJ, Lawlor DA, Matijasevich A, Horta B, Anselmi L, Araujo CL et al. What are the causal effects of breastfeeding on IQ, obesity and blood pressure? Evidence from comparing high-income with middle-income cohorts. Int J Epidemiol2011; 40: 670–680.
North K, Emmett P. Multivariate analysis of diet among three-year-old children and associations with socio-demographic characteristics. The Avon Longitudinal Study of Pregnancy and Childhood (ALSPAC) Study Team.
Eur J Clin Nutr2000; 54: 73–80. Holland B, Welch AA, Unwin ID, Buss DH, Paul AA, Southgate DAT. McCance and Widdowson's The composition of foods, 5th edn.
The Royal Society of Chemistry, Cambridge: London, UK, 1991. Tanner JM. Normal growth and techniques of growth assessment. Clin Endocrinol Metab1986; 15: 411–451. Clemons T. A look at the inheritance of height using regression toward the mean. Hum Biol2000; 72: 447–454.
Steer C. Comment:Clemons T-a look at the inheritance of height using regression towards the mean. Hum Biol2009; 81: 502. Taylor AE, Davey Smith G, Bares CB, Edwards AC, Munafo MR. Paterner smoking and maternal cotinine during pregnancy: implications for negative control methods. Drug Alcohol Depend2014; 139: 159–163.
Patrick DL, Cheadle A, Thompson DC, Diehr P, Koepsell T, Kinne S. The validity of self-reported smoking: a review and meta-analysis. Am J Public Health1994; 84: 1086–1093. Bingham SA, Gill C, Welch A, Day K, Cassidy A, Khaw KT et al.
Comparison of dietary assessment methods in nutritional epidemiology: weighed records v. 24 h recalls, food-frequency questionnaires and estimated-diet records.
Br J Nutr1994; 72: 619–643. Willet W, Stampfer M. Implications of total energy intake for epidemiologic analysis. In: Willett W (ed). Nutritional Epidemiology, 2nd edn. Oxford University Press: New York, NY, USA, 1998; 273–301. Leary SD, Davey Smith G, Rogers IS, Reilly JJ, Wells JC, Ness AR.

Smoking during pregnancy and offspring fat and lean mass in childhood. Obesity2006; 14: 2284–2293. Tulldahl J, Pettersson K, Andersson SW, Hulthen L. Mode of infant feeding and achieved growth in adolescence: early feeding patterns in relation to growth and body composition in adolescence.
Obes Res1999; 7: 431–437. Victora CG, Barros F, Lima RC, Horta BL, Wells J.
Anthropometry and body composition of 18 year old men according to duration of breast feeding: birth cohort study from Brazil. BMJ2003; 327: 901. Toschke AM, Martin RM, von Kries R, Wells J, Davey Smith G, Ness AR. Infant feeding method and obesity: body mass index and dual-energy X-ray absorptiometry measurements at 9-10 y of age from the Avon Longitudinal Study of Parents and Children (ALSPAC). Am J Clin Nutr2007; 85: 1578–1585. Yin J, Quinn S, Dwyer T, Ponsonby AL, Jones G.
Maternal diet, breastfeeding and adolescent body composition: a 16-year prospective study. Eur J Clin Nutr2012; 66: 1329–1334. Kramer MS, Matush L, Vanilovich I, Platt RW, Bogdanovich N, Sevkovskaya Z et al. A randomized breast-feeding promotion intervention did not reduce child obesity in Belarus.
J Nutr2009; 139: 417S–421SS. Yang Z, Huffman SL.
Nutrition in pregnancy and early childhood and associations with obesity in developing countries. Matern Child Nutr2013; 9: 105–119. Przyrembel H.
Timing of introduction of complementary food: short- and long-term health consequences. Ann Nutr Metab2012; 60: 8–20.
RESULTSWe selected 2548 Saudis, 1423 males and 1125 females, aged 18 to 60 years. A significant trend (p trend25 kg/m 2). Obesity and overweight were more prevalent in men than in women and was observed early in both genders, at the ages of 18–19 in men and 30–39 years for women. In the age range of 40–60 years, muscle mass dropped significantly ( P. The term “globesity” signifies that the epidemic of obesity has become worldwide.
The prevalence of obesity was steady until the 1980s, but has since increased dramatically throughout the world. According to the World Health Organization (WHO) in 2014, rough estimates of the number of obese adults worldwide were 600 million. Obesity is a serious problem because of the increasing possibility of a wide range of health consequences, including hypertension, insulin insensitivity, diabetes mellitus, cardiovascular disease, and distinct types of cancers.
The burden of medical costs for obese individuals are 30% greater than for normal-weight peers. Each 5 kg/m 2 increase in body mass index (BMI) results in about a 30% higher mortality rate. The risk of death increases by 20%–40% in overweight individuals, and it escalates to 200%–400% in obese individuals. Roughly, 3.4 million adults die annually due to overweight or obesity.Obesity in Saudi Arabia is a major public health concern; the country has one of the most rapidly increasing rates of obesity in the world. Western lifestyle behaviors and the consequent elevation in BMI in developing countries, including Saudi Arabia, can lead to an alarming epidemiological transition from communicable to noncommunicable diseases being the main causes of death. Studies in Saudi Arabia from the late 1980s through the mid-1990s reported a continual growth in the prevalence of obesity of about 20%.
– These studies showed that the prevalence of obesity in different regions of Saudi Arabia was estimated between 13% and 27%. In 2014, about 28.7%, or 3.6 million Saudis, were obese, ranging from 24.1% for men to 33.5% for women in different cities. Furthermore, a high frequency of overweight and obesity has been observed in younger Saudis, which may further increase the prevalence of obesity in the adult population over succeeding years. A recent study of 2382 young Saudis, aged 15 to 24 years old, showed that about 38.2% and 44% of men and women, respectively, are either overweight or obese. This proportion is expected to rise substantially by 2020, reaching 41% and 78% for men and women, respectively.To our knowledge, most studies are focused on the trend of overweight and obesity with over periods of time.
Harpenden Stadiometer Manual Meat Grinder
However, no detailed studies describe trends in obesity and adiposity parameters by different age groups in Saudi Arabia. Therefore, this study aimed to describe trends in the prevalence of overweight and obesity by age groups and gender in the western region of Saudi Arabia and to determine the effect of this trend on some anthropometric measurements. SUBJECTS AND METHODSThis cross-sectional observational study was conducted between March 2011 and February 2012 in major cities in western Saudi Arabia (Mecca, Al-Taif, and Jeddah). Saudis aged 18 to 60 years were selected by convenience sampling. Printed announcements were placed in universities, malls, and hospitals to inform individuals about this community-based study. Pregnant women and persons with disabilities were excluded. This study was accepted by the Ethics Committee of the University of Umm Al-Qura, and informed consent forms were signed by all participants before collecting the data.All anthropometric measurements were taken during face-to-face interviews by well-trained professional interviewers.
Harpenden Stadiometer Manual Meat Company
Measurements included height, weight, waist circumference (WC), and body composition while participants wore light clothing and were barefoot. Height was measured in centimeters using a Harpenden stadiometer (Holtain, Crymych, Wales, UK). WC was measured in centimeters at the midpoint between the last costal margin and the iliac crest, using a measuring tape. Weight and body composition analyses were obtained by using an Omron HBF-510 Body Composition Monitor device with scale (Kyoto, Japan).
The apparatus, with footpad and handlebar electrodes, estimates various body composition variables such as body weight, body fat percentage, visceral fat percentage, and skeletal muscle percentage. Body mass index (BMI) was calculated as kg/m 2, and then the following BMI groups were obtained: underweight (. RESULTSOur sample consisted of 2548 Saudis, 1423 males and 1125 females, aged 18 to 60 years. Males were about 55.8% of the total participants. Age bracket frequencies were unequal: 12% (n=306) aged 18–19 years, 60.3% (n=1536) aged 20–29 years, 16.4% (n=417) aged 30–39 years, and 11.3% (n=289) aged 40–60 years.
Overall, 29.2% (n=743, BMI ≤30) were overweight and 25.9% were obese (n=660, BMI ≥30). Almost 40% had a normal weight (39.4%, n=1004). The prevalence in obesity subgroups was 16.3% (n=415) for obese class-I, 6.5% (n=165) for obese class-II, and 3.1% (n=80) for obese class-III.The mean (SD) age for the whole sample was 29.1 (8.5) years; 29.7 (8.0) years for males and 28.3 (9.1) years for females. Mean values for BMI were overweight for males and females (27.6 6.8 vs.
25.7 3.9 kg/m 2). The mean WC, muscle mass, and visceral fat were significantly higher ( P.
Results are expressed as mean (SD). P value was determined by Mann-Whitney U test (Although the median is appropriate to report with the Mann-Whitney U test, the means are more comparable to other studies.)shows the prevalence of BMI categories and the corresponding ORs by gender. The prevalence of overweight and obesity in males was higher than in females (62.8% vs. Males were about 1.9 times more likely to be overweight compared to females (OR=1.9, 95% CI=1.56–2.3). The study results presented that prevalence of obesity in males was higher compared to females (29.3% vs. 21.7%), and males had a 1.8-fold higher risk of being obese than females (OR=1.82, 95% CI=1.48–2.22).
Approximately 18% of males had 1.76 times higher odds of being obese class-I than did females (95% CI=1.39–2.22). Furthermore, males were at higher risk to be class-II obese and class-III obese, approximately two times (95% CI=1.46–2.91) and 1.67 times (95% CI=1.05–2.67), respectively, more than females. However, females had noticeably higher prevalence of underweight (8.9% vs. 2.9%) and normal weight (45.9% vs. 34.3%) than males. ParameterMale n (%)Female n (%)OR (95% CI)BMI (kg/m 2)Underweight (males vs.
Females)41 (2.9%)100 (8.9%)0.43 (0.3–0.64) aNormal weight488 (34.3%)516 (45.9%)1Overweight (males vs. Females)477 (33.5%)266 (23.6%)1.9 (1.56–2.3) aObese class-I (males vs. Females)259 (18.2%)156 (13.9%)1.76 (1.39–2.22) aObese class-II (males vs. Females)109 (7.7%)56 (5%)2.06 (1.46–2.91) aObese class-III (males vs.
Females)49 (3.4%)31 (2.8%)1.67 (1.05–2.67) bObese (males vs. Females)417 (29.3%)243 (21.7%)1.82 (1.48–2.22) a. Underweight: BMI 40 kg/m 2, obese: BMI 30 kg/m 2.presents the trends of BMI, muscle mass, and adiposity parameters by age.
For both genders, BMI, WC, body fat percentage, and visceral fat percentage all increased significantly (p trend.05) increase appeared at the middle-aged period. Regarding WC, higher than normal values for males (90 cm) and females (80 cm) were detected in the 30–39 age group for both genders. Men showed higher than the normal values of mean body fat percentage (24) and visceral fat percentage (9) at the young adult age, whereas females showed higher than normal values for body fat percentage (36) at the young adult age and for visceral fat percentage (9) at the middle-aged period. Muscle mass decreased significantly ( P. Parameter18–19 years(n=128, males)(n=178, females)20–29 years(n=885,males)(n=651, females)30–39 years(n=246, males)(n=171, females) 40 years(n=164, males)(n=125, females)P valueP trendWeight (kg)Males72.8 (18)78.6 (18.1)82.5 (17.8)84.6 (16.3). Results are expressed as mean (SD).
P value was determined by Kruskal-Wallis. P trend was determined by Jonckheere-Terpstra test. Mean JT Statistic, males: 284477.0 (weight), 280497.0 (BMI calculated), 284477.0 (WC), 284477.0 (body fat%), 284477.0 (muscle%), 281680.5 (visceral fat); females: 191318.5 (weight), 187688.0 (BMI calculated), 191318.5 (WC), 191318.5 (body fat%), 191318.5 (muscle%), 188668.5 (visceral fat).The magnitude of association between BMI and age brackets was determined by ORs for each gender. Interestingly, overweight and obesity in females at 20–29 years showed no significant ORs compared to females younger than 20 years. At 30 years of age and higher, ORs increased significantly ( P.
DISCUSSIONIn 2014, WHO declared that the worldwide prevalence of overweight and obesity affected about 1.9 billion adults aged 18 years or older. Overweight and obesity have increased continuously with time in Saudi Arabia and other Gulf countries. Our results showed that BMI and anthropometric indices were greatly influenced by age and gender. Significant trends (p trend3 servings/day, 23.1% vs. 15.5%, P200%) in both sexes, and women will exhibit more obesity than men particularly in the ≥35 age group. Ng et al, from their global estimation of overweight and obesity from 1980 to 2013, found that the peak age of obesity in developing countries was at about 45 years for men and 55 years for women.
From the previous results, the prevalence of overweight and obesity would be affected by the age of the sample; female weight gain could be higher than male weight gain at older ages. Because the majority of the sample was under 30 years old (n=1842; 72.3%), the prevalence of obesity is expected to be higher in men than in women, which was confirmed by the results of this study.The current study showed that WC and visceral fat were higher in males, but total body fat percentage was higher in females. This can be explained by the fact that fat distribution differs between males and females, the central obesity and apple-shape in men compared with the pear-shaped obesity in women.
Many other studies are in line with this finding., Body fat percentages differ among countries depending on genetic factors, eating patterns, regular exercise, and other life-style habits. A study in the United States (6544 men and 6362 women) showed that body fat percentages in males aged 18–29 years and 30–49 years were 26.6% and 30.6%, respectively; while the corresponding values in females were 24.5% and 31.5%, respectively. These results showed that body fat percentages in Saudi females were higher than that of American females, whereas Saudi males showed percentages similar to American males.
Another study in Kuwait showed that the average body fat percentages in males (mean age 39.1 years) and females (mean age 40.9 years) were 23.3% and 37.7%, respectively, which were relatively comparable to our results in Saudi Arabia. Furthermore, our study noted higher muscle mass percentage in men than in women, which could be related to a lower level and duration of physical activity among women in comparison to men, which is in accordance with the findings of the Memish et al, Al-Nakeeb et al, and Al-Dokhi studies. Indeed, the desert climate in Saudi Arabia presents a barrier for outdoor activity for both men and women. However, Moradi-Lakeh et al found that 42.8% of Saudi females were physically outdoor-inactive, whereas only 19.7% of males were physically inactive outdoors ( P.